Hi from Antarctica,
I know, few people can write to you from the land of ice. While many eyes are on COP28 in Dubai, I’d like to open a window on how European Focus works internally:
Every Wednesday online, we collaboratively discuss the topic on which we want to focus. And then, while I was on the ship in the Antarctic, our Hungarian colleague told us the story of Dániel Karsai, a man who brought his case about dying with dignity to the European Court of Human Rights, and how this could change the narrative about the ‘right to die’ in Hungary.
That’s our focus for this edition: when dying is not a private matter, but a societal issue, sometimes used by politicians as a tool in their propaganda machine. And how, even though the topic touches ethical issues, that doesn’t mean that it shouldn’t be addressed. From the ‘never-ending question’ in the Netherlands to an ‘ethical vertigo’ in France, it is an opportunity to reflect on this difficult question.
Alicia Alamillos, this week’s Editor-in-Chief

“I have no idea. This is a party you can only attend once,” 46-year-old constitutional lawyer Dániel Karsai answered journalists, when they asked him about his future. A future that, in his case, will last no more than a few years, leading to total paralysis and loss of speech, while leaving his mental faculties intact, and inevitable death.
In 2022, Karsai was diagnosed with ALS, a rare genetic disease brought to the world’s attention by legendary physicist Stephen Hawking. While he may not live to Hawking’s age of 76, he is using the time he has left to fight for the right to die, or, in his own words, “To die like the trees, standing”.
Hungarian law allows terminally ill patients to refuse life-saving treatment, but this does not apply to people suffering from ALS, as there is no treatment to refuse. If he wanted to travel to Switzerland, where euthanasia is legal, to end his life, even family members driving him there could be imprisoned on their return to Hungary.
Besides, Karsai does not wish to die in a room overlooking the Swiss Alps.
“If they teach us in school: ‘here you must live and die’ [in a poem by Vörösmarty Mihály], at least let me do it with dignity”.
As one of the most successful human rights lawyers in Hungary, he has represented hundreds of clients before the European Court of Human Rights. It is a dark twist of fate that he has launched a case for his own end-of-life decision in Strasbourg.
By sitting in a wheelchair in front of the panel of judges, he did much more than plead his case: he united a country torn apart by politics. Dying – he admits – “sucks”, but nobody can avoid it. To his surprise, Hungarians rallied behind him. From doctors to priests to philosophers, many have understood that Karsai is fighting for them all.
Should his case succeed in Strasbourg, the government will be obliged to change the law, making his struggle for human rights immortal.
France has been examining whether to change its law on euthanasia. Denis Berthiau, a lecturer at Université Paris-Cité, specialising in Bioethics Law, looks into this issue.
What is the situation regarding the right to die in France?
More than a year ago, Emmanuel Macron expressed the desire to change the current law (euthanasia as active assistance in dying is still prohibited by the Penal Code). To this end, a citizens’ convention was convened in early 2023.
It came to two conclusions. On the one hand, it recognised the need to improve dying in France by guaranteeing better access to palliative care. On the other, it recognised the need to take into account certain situations in which requests for assistance are made, and to develop a legal framework for assisted dying, either in the form of assisted suicide or “euthanasia”.
What’s the difference between “assisted suicide” and “euthanasia”?
With “assisted suicide”, the patient initiates the act that causes their death. In this sense, it is indeed a suicide. In “euthanasia”, the lethal act is carried out by the doctor and his team. It always takes place at the patient’s request, in the framework of medical assistance in the dying process. The difference, then, lies in the degree of medical involvement in the act of accompanying a patient to death. And it is precisely this point which is undoubtedly delaying the government’s project.
Macron speaks of an “ethical vertigo” regarding this issue. Why?
Most medical issues provoke an “ethical vertigo”. Reducing end-of-life issues to whether or not to allow euthanasia or assisted suicide is far too simplistic. But it is certain that the new law will not solve all the problems. It will only benefit a few people. The vast majority of patients do not want to hasten their death. Nor will the law concern people at the end of their lives who are incapable of expressing their wishes. But the fact that the ethical challenge may seem vertiginous doesn’t mean we shouldn’t tackle it.

Dr. Paul Tammert thought he had found a loophole in Estonian law, allowing him to perform assisted suicide. He even presented a gas-based device on an evening TV show that provided this service.
Two of his patients ended their lives using it, but a third attempt stalled as the machine ran out of gas. While he drove to another town to procure more lethal gas, the police arrested him. He is now on trial for illegal business activities.
While Tammert will be punished for his amateurish stunt, three quarters of Estonian doctors think there should be legislation for the currently unregulated ‘right to die’.

Euthanasia, or a ‘good death’, is a heated topic in the Netherlands, which is known for its liberal views. The Dutch approach reflects a strong belief in freedom and personal choice. The Netherlands was the first country to legalise euthanasia in 2002, and has one of the most progressive euthanasia laws in the world.
Euthanasia is allowed under strict conditions: the patient must endure unbearable suffering with no prospect of improvement, the request must be voluntary and well-considered, and the patient must be fully informed. The decision must be supported by at least two doctors to ensure a thorough and ethical process. The same criteria apply to euthanasia for patients who suffer unbearably from dementia or for psychiatric reasons, such as major depression or personality disorders, which are rare and subject to strict safeguards.
However, the debate doesn’t stop there. A social and political discussion is currently underway about extending the right of euthanasia to the elderly who feel their lives are complete, even in the absence of severe illness. This is groundbreaking, even for the Netherlands.
Critics worry this could put pressure on older people, who feel they are a burden, to choose euthanasia. Supporters argue that it’s all about personal freedom: a person’s sense of a fulfilled life, devoid of suffering, should be respected and the right to a dignified end is a fundamental aspect of personal freedom. Research commissioned by the government found that over 10,000 Dutch people aged 55 and over (out of 21,000 participants in the study) would consider euthanasia when they feel their lives are completed.
This debate shows how the Netherlands continues to push the boundaries when it comes to personal freedom. It’s a complex issue, as it highlights the delicate balance between safeguarding vulnerable individuals and honouring the deeply-held Dutch value of self-determination. As this debate continues, the Netherlands remains at the forefront, navigating the complex interplay of ethical, moral and personal freedoms.
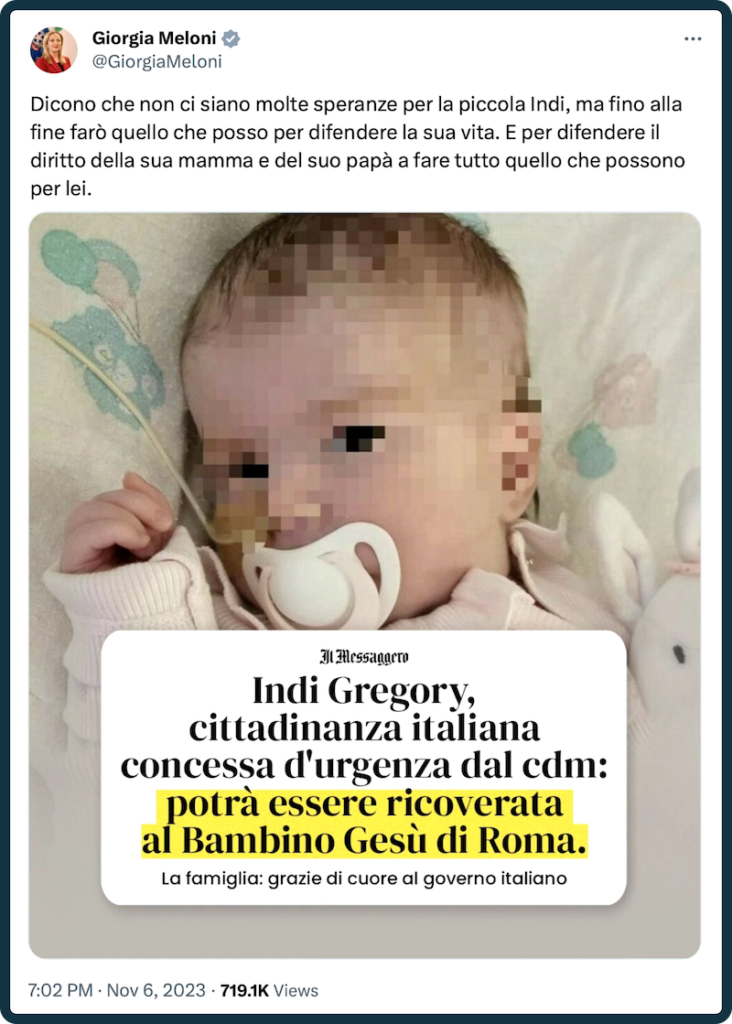
“I will do all I can to protect little Indi’s life,” Italy’s prime minister Giorgia Meloni tweeted, along with a picture of the eight-month-old Indi Gregory, an English baby girl with an incurable mitochondrial condition. Doctors and UK judges repeatedly said there was no way to save the baby, but the family had been fighting to keep the girl’s life-support machine running.
As part of her pro-life narrative, Meloni jumped on the story: she offered Italian citizenship to the baby, and to bring her to Italy before her life support was removed. British judges described Italy’s intervention as “wholly misconceived”. The baby died in mid-November, a week after this tweet.
After Indi’s death, Meloni has kept on posting her support for pro-life organisations. Even before taking over the government, Meloni’s far-right party limited the right to abortion in the Marche region, which is run by her party, Brothers of Italy.
Thanks for reading the 55th edition of European Focus,
How to die is a difficult question in our societies, and it has to be considered from many different perspectives, from the legal to the medical, social or even religious.
European countries are now thinking about this at both an individual level, and transnationally, as we do in this issue of European Focus. Let’s see what we discuss next time.
See you next Wednesday!
Alicia Alamillos






